The scars left by adverse childhood experiences CAN be healed
Recently, the topic of Psalm 23 came up in a conversation I was having with a client who is going through a ‘dark night of the soul’. Even if you’re not a regular church-goer, you’ve almost certainly encountered this moving poem about the faith that carries the psalmist (traditionally held to be King David) through challenge and suffering:
The Lord is my shepherd; I shall not want.
Psalm 23 (King James version)
He maketh me to lie down in green pastures: he leadeth me beside the still waters.
He restoreth my soul: he leadeth me in the paths of righteousness for his name’s sake.
Yea, though I walk through the valley of the shadow of death, I will fear no evil: for thou art with me; thy rod and thy staff they comfort me.
Thou preparest a table before me in the presence of mine enemies: thou anointest my head with oil; my cup runneth over.
Surely goodness and mercy shall follow me all the days of my life: and I will dwell in the house of the Lord for ever.
Later that day, my client sent me the following text from a commentary on Psalm 23 by Brother Fredrick-James:
…notice the words of the psalmist [who] is not stuck in the valley,
the psalmist is not wallowing in the valley,
they’re not lost in the valley,
they’re not setting up camp in the valley,
they haven’t stopped in the valley,
they’re not trying to get out of the valley or giving up in the valley,
the psalmist says that they are walking through the valley.
Brother Fredrick-James’ emphasis on “walking through” as the only spiritually healthy way to deal with one’s suffering (rather than either attempting to evade it, wallowing in it, or giving up in the face of it) is, of course, metaphorical. But according to recently-published research in the journal Biological Psychiatry: Cognitive Neuroscience and Neuroimaging, there may be literal truth to the psalmist’s guidance as well: Physical activity rewires the brain in people who suffered childhood adversity, making them more resilient to stress.
The background to this study is that adverse childhood experiences – emotional abuse, physical abuse, sexual abuse, emotional neglect, and physical neglect – are associated with an increased risk of both physical illness (including cardiovascular disease, diabetes, asthma and chronic pain conditions) psychological disturbances (including depression, posttraumatic stress disorder and anxiety), in adulthood.
This increased propensity to chronic ill-health is linked to long-term alterations in brain function, dubbed “neurobiological scars”. Put simply, adverse childhood experiences ‘rewire’ the brain, causing maladaptive changes to the stress response and to the immune response to infection and injury, and these changes can lead to illness in both the body and mind.
So, does that mean that if you had a rough childhood, you’re totally screwed? Not so fast. Childhood abuse and neglect increase the risk of going on to develop chronic illness; they don’t make it a certainty. And that observation leads to some intriguing questions: What’s different about the people who suffer impaired health attributable to adverse childhood experiences, vs those who don’t? Are there modifiable factors that prevent those neurobiological scars from developing, or that help them heal?
One very obvious candidate is physical activity. Exercise powerfully promotes neuroplasticity, the ability of the brain to rewire itself in response to experience. When we exercise, a cocktail of chemicals is released by our muscles, heart, lungs, fat tissues… and also by the brain.
Brain-derived neurotrophic factor (BDNF), glial cell line-derived neurotrophic factor (GDNF) and nerve growth factor (NGF), secreted in response to exercise, are all linked to increased cell growth and proliferation within the brain and central nervous system, and to synaptic plasticity, which is the ability of neurons to form new connections with each other and to weaken or break other connections.
There’s tantalising evidence that in adults with a history of adverse childhood experiences, those who were physically active might have fewer physical and psychological symptoms.
And the researchers behind this new study had already reported that the amygdalas of survivors of adverse childhood experiences with low lifetime physical activity were enlarged, while those with high lifetime physical activity were not. The amygdala is a tiny almond-shaped region of the brain that is often described as the fear response centre. It plays a key role in emotion processing and salience detection (filtering incoming stimuli to decide what to pay attention to), and is believed to be critically involved in the development of anxiety disorders such as posttraumatic stress disorder.
The next step was to investigate whether the level of physical activity throughout the lifespan affected communication between the amygdala and two other brain structures involved in processing emotions: the hippocampus, which is involved in encoding memories, and the anterior cingulate cortex, which plays a key role in emotion regulation.
To do this, the researchers examined resting-state functional magnetic resonance imaging (fMRI) data from 75 German adults with a history of childhood adverse events. fMRI measures activity levels in regions of the brain, by detecting changes associated with blood flow. It can also identify brain regions that are functionally connected, as these will ‘light up’ at the same time.
The crossover effect
Analysis of the fMRI data in conjunction with the participants’ self-reported lifetime physical activity levels revealed an intriguing finding:
Adults who had endured more adverse childhood experiences had less connectivity between the amygdala and anterior cingulate cortex if they had been less physically active throughout their lives, but more connectivity if they had been more active. The figure below illustrates the relationship between amygdala-anterior cingulate cortex connectivity and lifetime physical activity level:
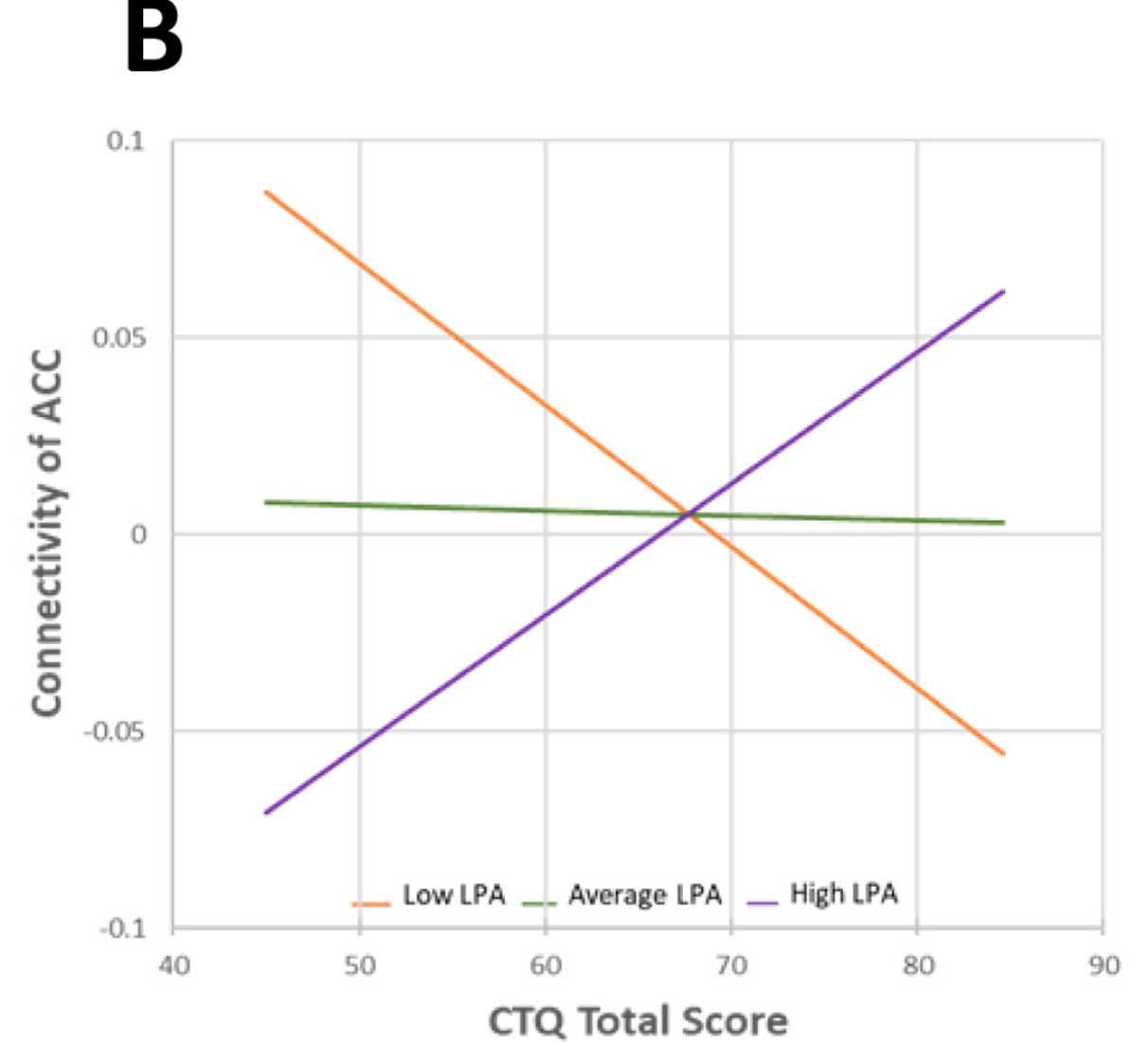
The researchers concluded that
“Higher activity levels were linked to connectivity profiles consistent with potential neural resilience to early adversity. These findings highlight physical activity as a modifiable lifestyle factor associated with neurobiological adaptation following early adversity.”
How much exercise is enough… and is there such a thing as too much exercise?
What exactly does “higher activity levels” mean? The researchers identified a “sweet spot” of between 150 and 390 minutes of physical activity per week as being optimal for promoting neural adaptation. They cautioned that some individuals may use excessive exercise as a maladaptive coping strategy, exhausting themselves in order to drown out their distress.
But within sensible bounds, maintaining higher levels of physical activity throughout life helps to heal the neurobiological scars inflicted by adverse childhood experiences, and nurtures both physical and psychological resilience to the many stressors that will inevitably be encountered throughout life.
So, whenever you find yourself walking through the valley of the shadow of death, the trick to surviving, and even thriving, is to keep walking.



